Large Practice
At RevlyticsHealth, we help large practices simplify billing, ensure compliance, and optimize revenue cycle management—so your team can focus on delivering quality patient care.
- Home
- Large Practice
Large Practices Pursue Similar Aims
- Shared Goal: Revlytics Healthcare and large practices both prioritize providing high-quality healthcare.
- Efficiency and Performance: Both entities aim to optimize operational efficiency and financial performance.
- Patient Focus: Both entities prioritize patient care and satisfaction.
- Regulatory Compliance: Adherence to industry regulations is a shared goal.
- Collaboration Benefits: Working together can enhance the overall quality and accessibility of healthcare services.
Faster cash receipts
Error-free billing & coding
Enhance patient satisfaction
Cost-effective solutions
Complete denial resolution
Adherence to regulations

Our medical billing services feature a strong and reliable billing infrastructure
Large practices face many challenges, including managing multiple claims. This can be time-consuming and complex, requiring careful attention to detail and adherence to regulations.
Our robust billing infrastructure offers transparency, affordability, and flexibility, addressing the shortcomings of traditional billing processes.
Revlytics Healthcare provides efficient billing services, backed by up-to-date denial management resources and experienced personnel, offering solutions and round-the-clock support.
Medical billing solutions to optimize revenue cycle management for large practices
Eligibility check
Secure pre-approval and confirm insurance eligibility for medical services, such as diagnoses, procedures, and treatments.
Patient Registration
Gather, verify, and accurately input data into the system to ensure error-free billing documentation.
Claims Submission
Our 99% clean claim rate ensures accurate claim submissions, maximizing your first-time pass rate and collection rate.
Coding & Documentation
Our team of expert coders and billers ensures accurate diagnostic and procedural coding.
Denial Management
Correcting the root causes of denials leads to improved accuracy and successful denial management.
Payment posting
We record payments from insurers or patients and inform patients about any co-payments.
A/R Follow-up
We follow up on overdue payments and accounts receivable to maximize collections.
Patient Billing
We ensure that patients are charged accurately for the services they have availed.
8 vital KPIs to expedite return on investment
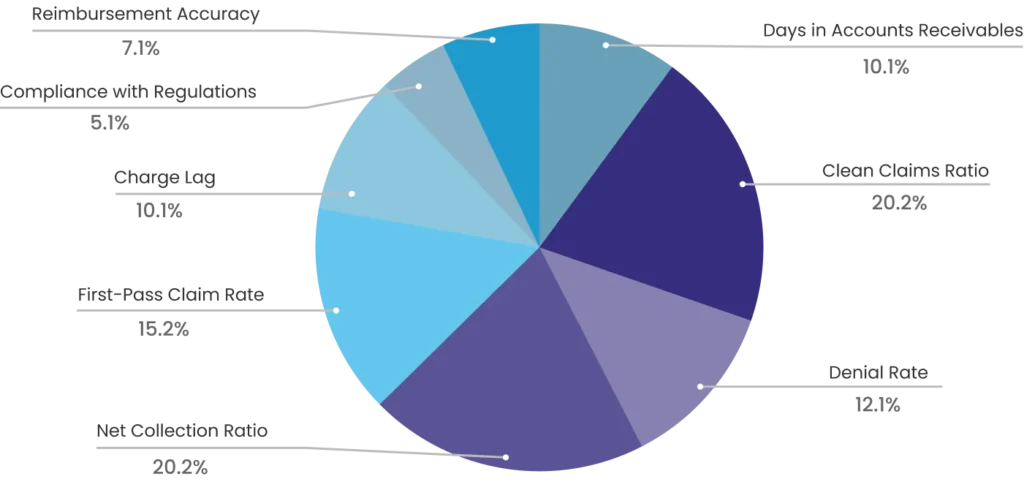
Elevate your billing, coding, and RCM performance with customized medical billing solutions
At RevlyticsHealth, we understand that one-size-fits-all solutions don’t work for every healthcare practice. Your large practice has unique needs, and we are committed to providing customized billing services that are transparent, accurate, and efficient.
Our team conducts thorough audits of your billing process to identify and rectify errors. We also focus on resolving unpaid and aging claims, helping you improve your cash flow.
We recognize that large practices face numerous challenges, from patient registration to claims submission and denial management. Our goal is to alleviate your non-clinical burdens, allowing you to focus on delivering exceptional patient care.
RevlyticsHealth offers comprehensive billing, coding, and RCM solutions tailored to your practice’s specific needs. We have a proven track record of submitting clean claims over 99% of the time, ensuring timely submission of medical claims, following up on aging accounts receivable daily, and increasing reimbursements.
Our efficient processes expedite our ability to reach these objectives
24/7 Access to Technology and Infrastructure
RevlyticsHealth offers cutting-edge billing technology, coding tools, and infrastructure that enhance operational efficiency and provide personalized billing and RCM solutions for large practices. Outsourcing billing to us allows you to leverage these resources without the overhead of software or hardware costs.
Upfront Communication
Effective communication between insurers, administrative staff, and billing personnel is essential for building strong, lasting partnerships. It fosters trust and minimizes misunderstandings and errors.
Regular Auditing & Quality Control
We ensure regular internal audits to scan inaccuracies and point out areas for improvement in the billing processes. Not only that, we rectify the patterns and ensure quality control measures, such as double-checking claims and conducting reviews. This allows a reduction in revenue holes and inaccuracies.
Simplifying Complex Coding System (ICD-10, CPT, HCPCS)
We prioritize staying informed about the latest regulatory changes, coding guidelines, and insurance requirements. Our team of skilled coders, proficient in ICD-10, CPT, and HCPCS coding systems, ensures accurate coding and faster collections.
Expertise & Specialization
Our team's experience and professionalism are key to reducing denials. By outsourcing billing to us, your large practice can access this expertise and ensure compliance with billing regulations.
Dedicated Account Management
RevlyticsHealth provides dedicated account managers who act as a single point of contact for your practice. This ensures personalized support, quick issue resolution, and smooth coordination between your staff and our billing team, leading to improved efficiency and stronger partnerships.

